Evidence-Based Upper Limb Retraining
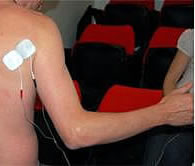
Is there evidence to support the routine use of functional electrical stimulation (FES) after stroke to reduce shoulder subluxation and elicit muscle recovery?

Is there evidence to support the use of prolonged low-load stretches or splints for the prevention of muscle contracture after stroke?

What evidence is there for eliciting muscle activity in paralysed muscles?
This workshop focuses on helping therapists to minimise upper limb impairments post-stroke, and increase engagement in activities.
Course notes and content will be based on published research and movement science/motor relearning.
Published content on ‘Optimizing motor performance and sensation after brain impairment’ is available in both English and Chinese from our Resources page
This workshop is now run over 3 days and accepts 24 registrants
Target audience
The workshop will be of interest to occupational therapists and physiotherapists from hospital and community based settings, who teach adults following stroke and acquired brain impairment, as well as university lecturers. The workshop focuses on upper limb rehabilitation.
Pre-reading
will be provided to the organising group for distribution to participants
Learning Objectives
At the end of the workshop, participants will be able to:
Name
the essential components (invariant kinematic features) of normal reach and manipulation.
Recognise
common compensations when observing people with stroke/brain injury attempting to reach for and use everyday objects; understand and explain why these compensatory strategies should be discouraged during practice.
Discuss
factors thought to contribute to the development of muscle overactivity/spasticity, and strategies to prevent these secondary problems.
Explain
the relationship and differences between spasticity/overactivity, muscle length changes, missing essential components and compensations.
Plan and conduct
an observational analysis and motor training session with a person who has had a stroke
Name
key factors that affect motor learning, and how these factors can be modified to enhance learning and increase intensity of practice.
Use
an electrical stimulation machine to stimulate paralysed muscles.
Discuss
evidence related to various interventions including constraint-induced movement therapy and mirror therapy to improve motor recovery and function of a person’s upper limb.
Presenters
Workshop Timetable
| Time | Day 1 |
|---|---|
| 8.00 | Housekeeping, introductions; workshop overview |
| 8.30 Session 1 |
Analysis of normal movement: Essential components of reach and grasp (cup, pen, cutlery, brush). Anatomy revision. |
| 10.00 | Morning Tea |
| 10.20 Session 2 |
Analysis of Abnormal Movement: Missing components and compensations with videos. Allocate groups. |
| 12.15 | Lunch |
| 1.00 Session 3 |
Being an Effective Coach 1: Focus on goal setting, feedback, practice intensity and measurement, with feedback video. |
| 2.15 Session 4a |
Demonstration 1: Analysis and training of stroke participants 1 and 2; provision and set-up/video of overnight practice by tutors |
| 3.15 | Afternoon Tea |
| 3.30 Session 4b |
Demonstration 2: Analysis and training of stroke participants 3 and 4; provision and set-up/video of overnight practice by tutors |
| 4.30 | Large group discussion and questions. Evaluation form. Round robin with each person stating “One thing I learnt today…..” |
| 5.00 | FINISH |
| Time | Day 2 |
|---|---|
| 8.00 Session 5 |
Implications of evidence for clinical practice: A case example. Muscle length changes and spasticity. Interventions including stretching, splinting, casting, positioning and botulinum toxin |
| 9.30 Session 6 |
Training Ideas and Being an Effective Coach 2: With videos |
| 10.10 | Morning Tea |
| 10.30 Session 7 |
Training Ideas / Being an effective Coach 2 (continued) Setting up the Physical Environment to Optimise Practice: Videos /practical |
| 12.15 | Lunch |
| 1.00 Session 8a |
Clinical Session 1: Review practice and homework from Day 1 with 4 stroke participants (by tutors). |
| 1.40 | Groups meet for 15-20 mins to plan for Clinical Session 2 (eg Equipment needed; tasks to analyse; sequence of coaches) |
| 2.00 Session 8b |
Clinical Session 2: Groups assess /analyse (20-30 mins) together, then take turns training a new stroke participant. Aim for 300 repetitions. Write up /video overnight practice for hospital/home. |
| 3.30 | Working afternoon tea – Meet in small groups to discuss session, including coaching |
| 4.00 | (Evaluation form). Meet for debrief and discussion as a large group. Round robin with each person stating ‘One thing I learnt today….” |
| 4.30 | FINISH |
| Time | Day 3 |
|---|---|
| 8.00 Session 9 |
Evidence of Therapy Effectiveness -Lectures interpersed with videos and practical: (i) Electrical stimulation (ii) Mental practice |
| 10.15 | Morning Tea |
| 10.30 | Session 9 continued – (iii) Constraint therapy (iv) Mirror box therapy |
| 12.15 | Lunch |
| 1.00 Session 10a |
Clinical Session 3: Groups review practice and goals for stroke participant from Day 2. Re-measure performance. Progress practice. |
| 2.00 | Stroke participants have a short break. Groups provide verbal handover to the next group, including suggestions for training. Plan tasks to analyse, equipment needed and sequence of coaches |
| 2.15 Session 10b |
Clinical Session 4: Groups analyse and train another stroke participant. Aim for 300 repetitions. Audio-record coaching. Observe and record other coaches giving feedback. Set-up /video take-home practice. |
| 3.00 | Working afternoon tea – Groups meet to discuss session including coaching |
| 3.30 | Discussion as a large group/ Qs arising over 3 days. Statement of goal intentions. Evaluation form. Round robin with each person stating ’When I return to work next week, one thing I will do is ….” |
| 4.00 | FINISH |


